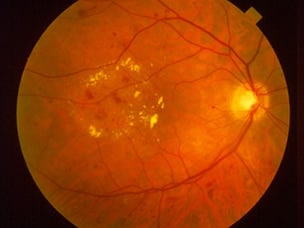
Diabetic Retinopathy
Diabetic retinopathy is the most common eye complication of diabetes and is a leading cause of blindness in adults. Diabetic retinopathy develops as a result of chronic elevation of blood sugars which then damages the internal lining of small retinal blood vessels. Damaged retinal blood vessels then are prone to leaking. This can lead to macular edema and vision loss. As blood vessels get progressively damaged from elevated blood sugars, these retinal vessels can also become blocked. This leads to a depletion of good blood flow to the retina. The retina then releases chemical signals to grow new blood vessels to feed itself (Proliferative Diabetic Retinopathy). However, these new blood vessels themselves are fragile and prone to breaking which can then cause vitreous hemorrhages and sometimes severe loss of vision. Tractional Retinal Detachments can also result from growth of these abnormal blood vessels.
Patients who develop diabetic retinopathy may initially not notice any change in their vision. But in its advanced stages, the disease can cause blurred or cloudy vision, floaters and blind spots – and, eventually, blindness. This damage may become irreversible without treatment.
Early stages of diabetic retinopathy do not usually require any treatment but patients must keep strict control of their blood sugar level to prevent the disease from progressing. If the disease does progress, treatment by a retinal specialist may be necessary to preserve your vision. The two most important causes of vision loss are now discussed below.
Diabetic Macular Edema
Treatment for diabetic macular edema typically involves one of the following options: observation alone with better control of blood sugars, ocular injections of medications, or the use of a laser. If a patient has significant macular edema, then injectable medications can slow or halt the release of fluid out of injured diabetic retinal blood vessels and thereby reduce macular fluid and improve vision and prevent vision loss. Available injectable drugs that do exactly this include: Avastin™ (off-label), Lucentis™ , Eylea™, biosimilar agents, Eylea HD™, Vabysmo™, and intra-ocular steroid formulations (Ozurdex™, Iluvien™). This list will continue to grow as we advance the field of retinal care.
Injectable treatments may require initial monthly injections to reduce diabetic macular edema and hence allow the macula to dry and you to see better. Injections can be spread out beyond 1 month as the macula responds to therapy. Because diabetes itself is a chronic disease, steady ongoing retinal therapy however, may be needed indefinitely to prevent you from experiencing vision loss over time. Our retinal practice can discuss the risks and benefits of injectable therapies. The best way to prevent damage from diabetic retinopathy is always to maintain an excellent Hemoglobin A1C and you must address this with your primary care physician or endocrinologist.
Another adjunctive category of treatment for diabetic macular edema is: Subthreshold Micropulse Laser. During this procedure, small laser spots are placed in the macula to limit leakage from damaged capillaries and also stimulate the removal of fluid out of the retina. The reduction in macular fluid will improve the function of the retina and help prevent vision loss and, in certain patients, even improve vision. Focal laser treatment is performed in our office under topical anesthesia and repeat treatments may be necessary to stabilize your disease.
Dr. Ilyas was one of the first retina surgeons in the region to offer a unique macular laser called “Micropulse Laser Therapy” (Iridex IQ 577 ™) for treatment of diabetic macular edema. Micropulse Laser can be useful to treat patients with Diabetic Macular Edema while preserving the health and well-being of the macular tissue. Micropulse laser works by chopping a continuous wave of laser into tiny low energy pulses with rest periods in between that spares the retina injury while treating the macular edema and reducing it.

The idea of a “gentler” laser therapy for treating diabetic macular edema as opposed to conventional thermal laser has generated a lot of interest in exploring this as a unique therapy for some mild cases of diabetic macular edema or even as an adjunctive therapy that can be coupled with injections of medications (see above) for even greater benefit on treating diabetic macular edema. Micropulse Laser therapy is also utilized in the treatment of several other retinal diseases including Central Serous Retinopathy. Dr. Ilyas has extensive experience in the use of the Micropulse Laser from Iridex.
Proliferative Diabetic Retinopathy
Treatment of Proliferative Diabetic Retinopathy often involves use of injections of medications into the eye (see diabetic macular edema drugs) and also the application of laser surgery called Pan-retinal or Scatter Laser Treatment. The laser treatments are used to shrink the newly developed blood vessels by applying laser burns in the peripheral retina. Scatter laser treatment is most effective before newly grown blood vessels have started to bleed, and may slightly reduce patients’ color and night vision, while preserving your central vision.
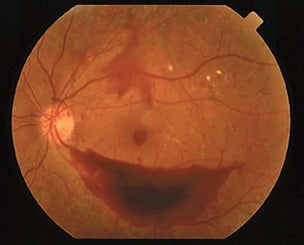
Severe vitreous bleeding may require surgery called vitrectomy, or removal of the vitreous, to remove blood from the center of the eye.
Left unchecked, Proliferative Diabetic Retinopathy can lead to tractional retinal detachments that can permanently disable the vision and cause eventual blindness. If the retinal detachment is severe enough, surgical intervention (vitrectomy with membrane peel) may be necessary to prevent total blindness. At Retina & Vitreous Consultants, we provide expert surgical care of these complex retinal detachments.
What can I do to prevent or limit my risk of Diabetic Retinopathy?
It is important for patients with diabetes to have dilated eye exams once a year to check for any signs of diabetic eye disease. You can also minimize your risk of developing diabetic eye disease by keeping your blood sugar and blood pressure under excellent control, eating a healthy diet, and exercising regularly.
To learn more about our Diabetic Retinopathy treatments and to find out if they are right for you, please call 540-662-1810 today to schedule a consultation.