An Epiretinal Membrane, also known as a Macular Pucker, is a thin layer of scar tissue that forms over the macula, the area of the retina that gives us clear central vision. An epiretinal membrane most often develops with age, as the vitreous gel that makes up most of the eye’s volume thins and pulls away from the retina inducing microtrauma to the retinal surface. Other causes of epiretinal membranes can include: diabetic retinopathy and vascular occlusive diseases, uveitis, retinal detachments, and eye trauma among others. The damage caused to the retina by any of the above entities then leads to the formation of scar tissue on the macula. When the scar tissue contracts, the retina wrinkles or puckers and macular swelling can ensue, which then causes blurry or distorted central vision. Patients with an epiretinal membrane may experience difficulty seeing fine details and reading small print and may also see straight lines appearing as wavy ones. There may also be a gray area or blind spot in the center of your vision.
Most cases of epiretinal membranes do not progress and do not require treatment. The symptoms of distortion and blurriness are usually mild and patients are able to adjust to the vision changes without much impact on their daily lives. Noninvasive treatments such as eye drops or medications will not improve vision that is reduced from an epiretinal membrane. If vision distortion or blur is severe enough, a vitrectomy with delicate peeling of the membrane may be performed to repair this condition. Dr. Ilyas can further discuss the impact of your macular scar tissue on your vision and whether surgery is truly indicated for you.
Diagnostic Tests
Fluorescein Angiography
Fluorescein angiography is the practice of taking photographs of blood vessels inside the eye (an angiogram) with the help of a intravenous injectable contrast dye (fluorescein dye). These pictures help doctors evaluate the retina and diagnose and track problems such as: diabetic retinopathy, macular degeneration, abnormal vessel growth, and macular swelling, among many other diseases.
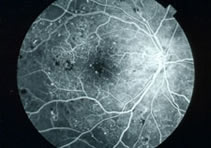
Initially, some pre-injection photos of the retina are taken with the camera (fundus Auto-Fluorescence images). The contrast dye is then injected in a small vein, usually in the patient’s arm. The dye travels up to the eye within seconds and “lights up” the blood vessels of the retina which allows the camera to capture the retinal circulation. Once the dye is injected, multiple photographs will be taken over the ensuing 10 minutes or so. The procedure is very well-tolerated in most patients and a discussion of the benefits and risks of the procedure will be shared with you on the date of your test.
OCT Imaging
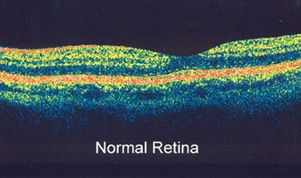
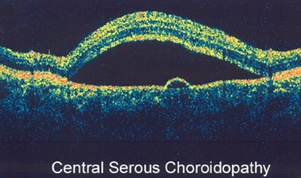
Optical coherence tomography (OCT) is an advanced diagnostic tool used to produce cross-sectional images of the retina and in particular the macula. These images can then help with the detection and follow-up of serious retinal conditions such as macular holes, macular edema, Wet Macular Degeneration, macular scar, and central serous retinopathy. OCT uses light rays to image the retinal layers in detail and does NOT involve any radiation exposure.
B-Scan Ultrasound of Eye
Ultrasound is a test that uses sound waves to assess the overall structural appearance of the vitreous and retina. If your doctor cannot view the retina because of something in the patient’s eye blocking the view (severe cataract or vitreous blood), then they can use ultrasound to determine the general status of the retina (e.g.- is there a Retinal Detachment back there?). B-scan US is also helpful for evaluating, measuring, and following tumors of the eye.
To learn more about retina and vitreous diseases and cutting-edge treatments available to you, please call 540-662-1810 today to schedule a consultation.